Just under 700 Filipinos were infected with HIV in October, based on the latest data from the HIV/AIDS and ART Registry of the Philippines (HARP) released by the Department of Health’s Epidemiology Bureau. For the month starting the last quarter of 2015, there were 651 new HIV Ab sero-positive individuals, a figure 21% higher compared to the same period last year.
Eighty-five percent (24,655) of all the 29,079 diagnosed cases in the Philippines were actually reported in the past five years, from January 2010 to October 2015.
According to Michael David dela Cruz Tan, publishing editor of Outrage Magazine, the country’s only exclusively LGBT publication that also has HIV-related programs, “we can give this a ‘positive’ spin – that is, more people are getting tested for HIV infection, so we now have a ‘clearer’ picture of the impact of the epidemic in the country.”
However, Tan said that “let’s be completely honest here: The continuing upward trend in the number of HIV infection in the Philippines highlights that our efforts – limited as they are – continue not to have the effects that we desire.”
For Fritzie Estoque, chairperson of the Misamis Oriental-Cagayan de Oro AIDS Network (MOCAN), “we were not surprised at all with the continuing steep upward trend. As a long-time advocate, together with my team, we have anticipated this trend to happen in the Philippines soon(er).”
Estoque said that MOCAN’s engagements and interactions with varied sectors of the society “gave us a picture of what’s going to happen in the next 10 years. Indeed, we are here now.”
Desi Andrew Ching, executive director of HIV and AIDS Support House (HASH), agreed, saying that “on a positive note, this is a sign that more and more people are becoming more educated, more informed and more aware about HIV and AIDS. It is a sign that more and more people are taking initiatives to reach more people towards informing and testing the at-risk population.”
However, the increasing number of people getting infected with HIV in the Philippines is “a realization that we are really far behind the other countries when globally… trends (show that HIV infection rates) are going down. We are among those with an aggressive increasing trend,” Ching said.
WORSENING PROBLEM
Among those who tested positive for HIV this October, 96% were male. The median age was 28 years old (age range: four years to 75 years). Half belong to the 25-34 age group, while 29% were youth aged 15-24 years old.
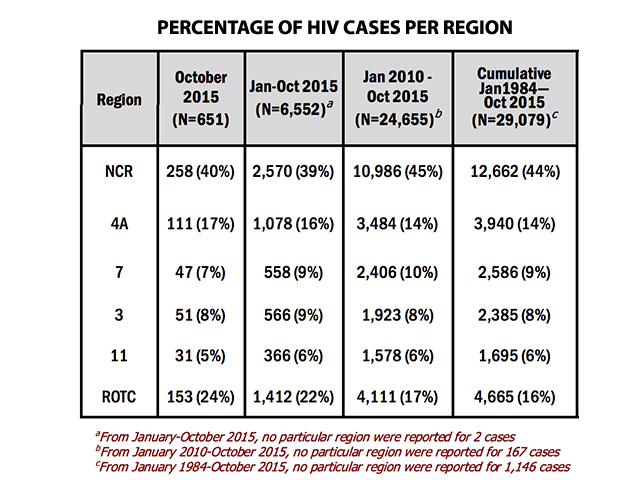
The regions with the highest number of reported cases for October were: National Capital Region (with 258 cases or 40%), Region 4A (111 or 17%), Region 3 (51 or 8%), Region 7 (47 or 7%), Region 6 (38 or 6%), and Region 11 (31 or 5%).
Reported modes of transmission were sexual contact (631), needle sharing among injecting drug users (IDU, 18), and mother-to-child transmission (2). Eighty-six percent of the sexually transmitted cases were among males who have sex with males (MSM).
According to Dr. Jose Narciso Melchor Sescon, who helms AIDS Society of the Philippines (ASP), “experts have predicted that HIV cases in the Philippines will continue to rise as a result of scaling up of access and availability of HIV testing and services across the country.”
Sescon, nonetheless, expressed alarm in “the trend (showing the rise in number of HIV infections). This should be taken seriously in terms of the scaling up efforts, as well as the setting of priorities (considering our) resources are still limited.”
Sescon also lamented the lack of political will in the country, particularly because many politicians and government officials ignore science-based solutions in the fight against HIV.
“We have yet to see political leaders with formidable conviction to support, implement and monitor effective programs, and even review and update the Philippine AIDS Prevention and Control Act,” Sescon said.
CHANGING TRENDS
How HIV is affecting Filipinos has been changing. From 1984 (when the first case was reported in the country) to 1990, 62% (133 of 216 cases) were female. Starting 1991, however, more males were reported to be infected with HIV in the Philippines. By the 2010-2015 period, males already comprised 95% (23,458) of the reported 24,655 cases.
Those who are getting infected are also getting younger. From 2000 to 2004, it was 30-39 years; from 2005 to 2009, it was 25-34 years; and from 2010 to 2015, it was 20-29 years. Data from the Department of Health’s Epidemiology Bureau showed that the proportion of PLHIV in the 15-24 year age group increased from 20% in 2005-2009 to 28% in 2010-2015.
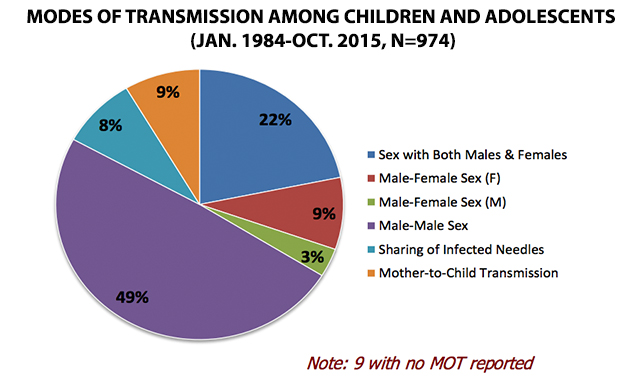
The modes of transmission have also been changing. While heterosexual sexual contact was the main mode of HIV transmission in the past, from January 2010 to October 2015, 84% (19,685) of infections through sexual contact were among MSM. Meanwhile, cases among IDU also increased from <1% in 2005 to 2009, to 5% within the past five years.
Outrage Magazine’s Tan also noted that “just as the country has been ill-equipped with responding to the link between drug use and HIV infection in the Philippines, we are now seeing the same lack of capacity in responding to the link between the sex industry and HIV infection.”
In the Department of Health’s October figures, 11% (73) of those who tested HIV-positive engaged in transactional sex; with most (97%) of them male whose ages range from 16 years old to 61 years old (median: 30 years). Fifty-five percent of males who engaged in transactional sex were the ones who paid for sex.
As defined, “people who engage in transactional sex are those who report that they regularly accept payment for sex, pay for sex, or do both.”
The Department of Health’s Epidemiology Bureau further reported that “a total of 2,399 cases reported… from October 2012 to October 2015 were people who engaged in transactional sex. Ninety-six percent were male. Of the 2,399 cases, 1,314 (55%) paid for sex, 707 (29%) accepted payment for sex, and 378 (16%) engaged in both.”
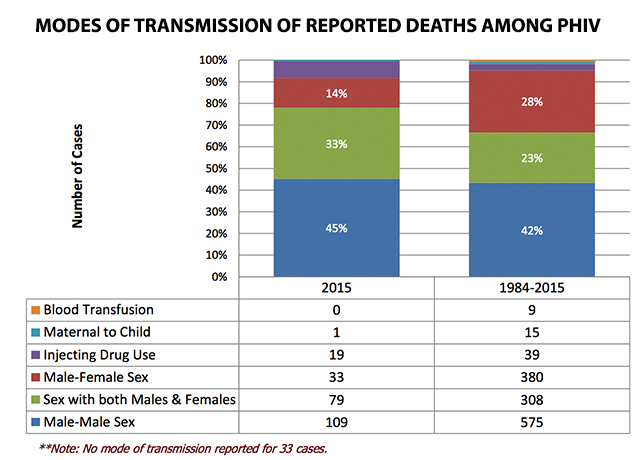
For the month of October, there were 50 reported deaths.
(EVEN) MORE TO DO
ASP’s Sescon said that “we still have a long way to go in terms of coverage (of HIV testing) and reaching of targeted populations at risk to HIV infection.” For Sescon, to broaden the scope of the existing efforts, “everyone has a responsibility to do; it has to begin with ourselves first.”
HASH’s Ching said that “there is a need to keep pushing for more information dissemination and more education in the community. More programs should be implemented from the grassroots level to strengthen new organizations working on HIV and AIDS. More campaigns should be conducted to promote prevention and early diagnosis and treatment. The youth should be engaged aggressively, considering that the age range of the newly affected are those from 15-24 years old.”
Ching also tasked the PLHIV community in dealing with HIV. “The PLHIV community should demand less and act more, expect less and move more. The health system has a long way to go from becoming at par with our neighboring countries, but other than a more progressive health system is the need for a more mature and more emphatic health service provider program.”
For Outrage Magazine’s Tan, “the solutions we provide to confront this problem should be holistic. Yes, we need to continue promoting means to prevent the spread of HIV – from intensifying campaigns for condom use, introduction of pre-exposure prophylaxis (PrEP) and post-exposure prophylaxis (PEP) in the Philippines, and inclusion of sex-positive messages in educating the public, among others.”
But Tan said that “we should not just ‘put all our eggs in one basket’ – as the saying goes – by over-emphasizing only prevention efforts.” As it is, Tan said that “the HIV discussion in the Philippines is often ‘dictated’, if not hijacked, by those who are not HIV-positive, so that the needs of PLHIVs are generally neglected.”
Tan added: “It is only right that we worry that the numbers of those getting infected with HIV continue to increase, just as it is right for us to take all steps to stop HIV infection. But we should also not forget that there are already so many Filipinos who are infected with HIV, and we need to better their access to quality treatment, care and support services. Solving this epidemic goes beyond people knowing their HIV status. It also means including PLHIVs in the conversations; and ensuring that their needs after they find out that they are HIV-positive are served.”
For Tan, efforts that need to be highlighted, include bettering “access to antiretroviral medicines, uniform implementation of PhilHealth coverage (since PLHIVs in different hubs receive different services, even if they pay the same premium), amendment of the Philippine AIDS Prevention and Control Act to ensure it protects the rights of PLHIV, and dealing with stigma and discrimination that many Filipinos living with HIV now face.”
MOCAN’s Estoque echoed the World Health Organizations’ call for a “bigger response” to bring the epidemic under control, “though, really, we should have next big STEPS.”
Like Tan, Estoque is calling for the “immediate amendment of Republic Act 8504 since there are provisions in this law that somehow hinders the prevention and control program of the government”; and the introduction of PrEP as another choice for HIV prevention.
But Estoque added that there is also a need for the Department of Health to “create/provide more timely training opportunities for dedicated advocates and active organizations to level-up their capabilities and potentials.; share the DOH’ technical support and resources fairly and justly without politics”; and not opt-out people in prison (PiP), women and other key affected populations in the services offered.
Meanwhile, local government units (LGU) “should come up with a functional and a working Local AIDS Council. An effective HIV and AIDS Ordinance should serve as a guiding principle in dealing issues re: HIV & AIDS in every LGU. Apart from treatment, care and support (TCS) and capability building mechanisms, a component on education and prevention and control program must also be given of equal importance. Awareness is power. One can have the power to choose the best option for his/her own health. Positive awareness can save one’s life,” Estoque said.
Estoque said that care should be given to those rendering services/frontline service providers. At least in MOCAN’s observation, site implementation officers (SIOs) and peer educators are not paid on time (delays taking up to four months), which – in turn – affects the quality of care provided by those in the frontline.
Estoque similarly recommended for the health sector to “improve quality service. This sector must not just perform their respective duties merely to comply the expectation and target accomplishments as required, but rather work as effective and as compassionate health providers always serving to the best interest of the patients. Serve with care and respect.”
“As for MOCAN, we continue to do all of these: correct misconceptions, educate properly both the young and general population in schools, in communities, in churches, and in different institutions. We continue to speak, collaborate, and engage with officials so that we can level up our campaigns. We continue to empower providers to give complete and genuine health care, eliminate stigma and discrimination. We continue to inspire more individuals, more organizations to help us deliver the message of hope. Hope that having an HIV is not a life sentence. Hope that there is life after getting infected with HIV. And that the hope is available and free (treatment) and if one seeks for that help voluntarily, we handle one with utmost confidentiality and respect,” Estoque said.
“The worsening HIV situation in the Philippines is highlighting how far we are from truly ending this problem,” Tan said. “And – sad as this may sound – if we continue doing only what we’re doing even if we know that they are not enough, then our situation will not change anytime soon.”