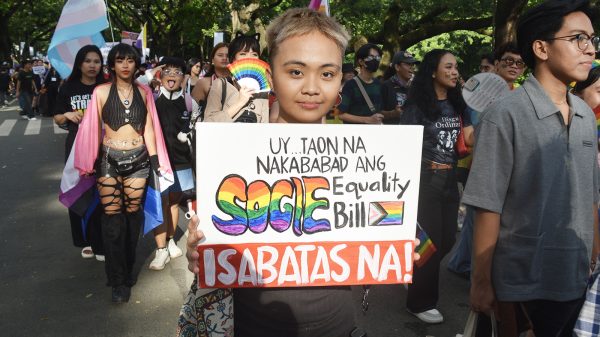LGBTQ2SPIA+ patients face unique cancer risks, including fear of discrimination, higher incidence of certain cancer sites, and lower screening rates, resulting in more cancers detected at later stages.
This is according to the Journal of Medical Imaging and Radiation Sciences, published by Elsevier, where undergraduate researchers from the University of Alberta’s Radiation Therapy Program in the Faculty of Medicine and Dentistry describe how the experience of LGBTQ2SPIA+ when dealing with cancer risks are different.
To discover the knowledge, attitudes, and practice behaviors of the healthcare professionals treating these patients, the authors surveyed Radiation Therapists (RTs)–key members of the cancer treatment team who are responsible for planning and delivering radiation therapy. In addition to the highly technical aspects of the job, RTs explain procedures, answer questions, comfort patients, and provide emotional support during the treatment journey, making these professionals a natural point of education and support for LGBTQ2SPIA+ patients.
Results suggest there are knowledge gaps and inconsistencies when caring for this patient population. Over 70 percent of respondents were unfamiliar with all terms associated with LGBTQ2SPIA+, and the same percentage were unsure if specific resources were available for the LGBTQ2SPIA+ population at their cancer center. This uncertainty affects the care given to these patients, either limiting RT’s interactions with this community or being unable to provide specific side effect management education, a crucial part of the RT role.
Despite clear evidence of the RT community desiring LGBTQ2SPIA+-specific care, a significant portion of respondents stated that all patients should be treated equally, and therefore no practice adaptation is required. Most respondents reported being comfortable caring for the LGBTQ2SPIA+ community, despite the majority also asserting that they have had inadequate education in this area.
However, the survey found an overall willingness to improve practice behaviors, with 86.9 percent of total respondents interested in receiving more education on this topic. As one respondent stated:
“I can’t really think of ‘how’ I am actively creating a safe environment for disclosing their sexual orientation, nor do I know how to properly create that environment….I can definitely say that I am non-judgmental of their life choices if it comes up in conversation, etc., but I really don’t know what more I should be doing, admittedly. Further training or information on how to better create a safe environment for patients would be beneficial.”
The authors conclude that future research should examine the experiences of LGBTQ2SPIA+ patients from their perspective. To provide truly patient-centered care, LGBTQ2SPIA+-targeted resources for both patients and radiation therapists need to be considered a priority.